Townsend Letter – The Examiner of Alternative Medicine
Cannabinoid Deficiency and Its Impact on Human Health and Disease, Part 3
by Jonn Desnoes, OMD, MD, PhD, and Sandra Kischuk, MSMIS, MCPM
Page 1, 2
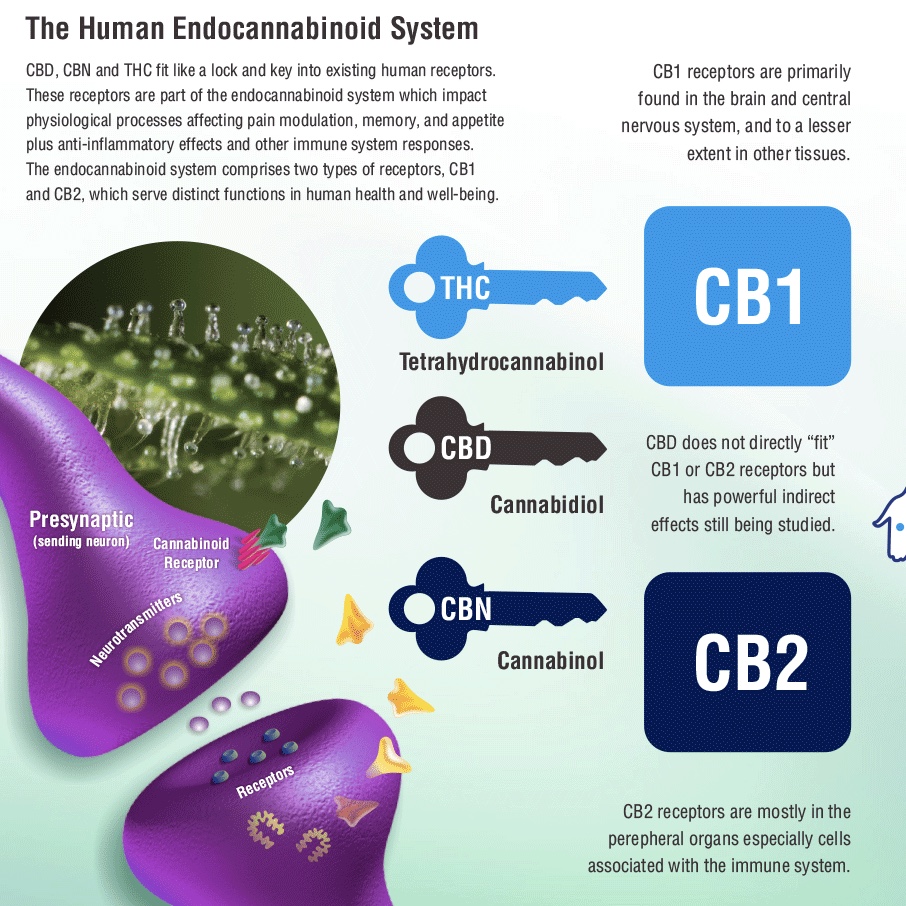
The Endocannabinoid System
The discovery of the endocannabinoid system not only changes our understanding of human body physiology, it is a game-changer in altering our approach to treating diseases and conditions we previously considered difficult or even impossible to control. Dr. Mauro Maccarrone, University of Teramo, Italy, describes the endocannabinoid system as the “guardian angel” of mammalian reproduction, with the endocannabinoid signaling system controlling the reproduction process – governing spermatogenesis, fertilization, transport of the zygote through the oviduct, implantation, and fetal development. Prolific placental CB receptors “pass messages” between the embryo and the mother. In maternal milk, endocannabinoids activate the newborn suckling response. A dysfunctional endocannabinoid system can be the underlying cause of colic. Israeli neuroscientist Ester Fride noted that No-CB-receptor mice suffered the same fate as human babies with “failure to thrive” syndrome – they weakened and died prematurely.1

Cannabinoid Therapies
PubMed, the US National Library of Medicine, National Institute of Health, lists over 1,200 research papers related to delta-9-tetrahydrocannabinol, 7,800 related to tetrahydrocannabinol, almost 15,600 referencing cannabis, over 21,000 which talk about cannabinoid, and over 1,500 with the term cannabidiol.
One example of a study that had both the terms cannabis and cannabidiol (CBD), “Cannabidiol rather than Cannabis sativa extracts inhibit cell growth and induce apoptosis in cervical cancer cells,” reached the conclusion that both concentrated cannabidiol (CBD) and crude (unrefined) Cannabis sativa extracts (the latter of which would have the full range of cannabinoids) “were able to halt cell proliferation in all cell lines (types of cervical cancers) at varying concentrations,” meaning that the cancer cells stopped growing and multiplying. They further revealed that apoptosis (cell death) was induced by cannabidiol.2 Stop the cancer cells from making new cells and kill the ones already there? Sounds like a great idea.
Researchers at St. George’s Hospital, University of London, evaluated the in vitro effect of six cannabinoids (two forms of cannabidiol [CBD], two forms of cannabigerol [CBG] and two forms of cannabigevarin [CBGV]), separately and in combination, on cancer (leukemia) cells. Conclusions:
1) Cannabinoids reduce cell number by being cytostatic. (stopping cell processes)
2) Cytotoxicity can be achieved through a break in treatment (recovery phase).
3) Cannabinoids alter cell signaling proteins.
4) CBD acts non-antagonistically with other cannabinoids to reduce cell number.
5) Cannabinoid activity is influenced by drug combination and treatment schedule.3
Cannabinoids, an amazing complex of biochemicals, support the homeostatic system of the human body. Homeostasis is defined as “A state of equilibrium, as in an organism or cell, maintained by self-regulating processes.”4 We can think of a human’s homeostatic system as a “regulator” that keeps the body’s physiological, chemical, and electrical systems in balance. Thus, we can see how a nutritional deficiency that affects the body’s homeostatic system can impact the entire body, causing problems ranging from aberrations at the cellular metabolic level (e.g., cancer and autoimmune diseases) to gross changes in physiological, mental, and emotional functioning. Cannabinoids provide vital nutrients necessary for the normal functioning of the human body and the prevention of disease.
Whether the result of poor diet, lack of exercise, drug abuse, environmental toxins or genetic factors, endocannabinoid deficits are associated with a reduced ability or inability to adapt to chronic stress. Prolonged exposure to stress depletes endocannabinoid tone, and this, in turn, has an adverse impact on a plethora of physiological processes. Ironically, the US government’s unending search for marijuana’s harmful properties yielded not only information about one of the human body’s most critical systems but also astonishing scientific insights that validate the herb’s therapeutic utility.
Sources of External Cannabinoids
Traditionally, hemp was grown for fiber and oil, but what is often overlooked is that hemp was used as livestock fodder for farm animals, including chickens, cows, goats, and pigs. Cannabinoids are lipids – fat soluble – and, once consumed, would be retained in the animals’ meat, dairy products, and eggs. People who ate animal products would get these residual cannabinoids.
A second source prior to 1937 were the many over-the-counter and prescription medicines that included hemp/cannabis products. A third source for those who grew hemp would have been through physical contact. Farmers who worked in the hemp fields would invariably brush against the plants, and, in all likelihood, absorb some of the terpenes, flavonoids, and cannabinoids through the oils that clung to their clothes and skin.
Interestingly, a centuries-old method of harvesting these oils, used in the Chu Valley between Kyrgyzstan and Kazkhstan, involves sending a clean and naked rider on a well-washed horse through the fields of an extremely potent variety of cannabis for a few hours, then scraping off the oily, sticky residue from both horse and rider. One might expect that, by the end of the ride, after breathing and wearing the oils for four hours or more, both horse and rider would be feeling no pain.5
The primary natural sources of cannabinoids are the two phytocannabinoid-rich botanicals, Cannabis sativa and Cannabis indica. A third variety of cannabis, Cannabis ruderalis, appears to be unimportant as a source of cannabinoids.6 Aside from cannabis, some other plants have small amounts of cannabinoids, which may or may not have affinity for human cannabinoid receptors. Four members of the Asteraceae flower family – Echinacea purpurea, Echinacea angustifolia, Helichrysum umbraculigerum, and Acmella oleracea (common name – toothache plant) – and a liverwort, Radula marginata,bear minor amounts of phytocannabinoids, predominantly, but not exclusively, in the roots and flowers. Yangonin, a chemical in the Kava plant, has a significant affinity for the CB1 receptor. Both human cannabinoid receptors respond to tea (Camellia sinensis) catechins, and black truffles contain anandamide. Whether the body has any way to use the cannabinoids in these herbs/mushrooms is not known, and it is unlikely that these alternative cannabinoid sources will be researched until all of the cannabinoids in cannabis have been thoroughly profiled.7
Transdermal Application
Because cannabinoids are lipophilic, transdermal application is an effective way to take cannabis, at least for some conditions.
Dr. Mark Sircus, Ac., ODM, DM(P), (acupuncturist, doctor of oriental and pastoral medicine and a well-known online doctor of alternative medicine) practices what he refers to as natural allopathic medicine. Allopathic medicine is what we think of as traditional medicine: where a doctor will treat a medical problem by writing a prescription for an FDA-approved chemical compound. Natural allopath? Natural prescriptions. Dr. Sircus, who claims 45,000+ followers, links his website (http://drsircus.com/medicine) to the source of a time-lapse video clip about covering skin sarcoma with a CBD oil patch and curing it in 35 days (http://CureYourOwnCancer.org). Melanoma took longer – 60 days.8
The skin is more permeable to cannabinol and cannabadiol than it is to THC, so patients who apply cannabis products to the skin are not likely to experience a dramatic THC high. Dr. Audra Stinchcomb, a researcher at the University of Kentucky, holds that transdermal patches are a preferred treatment method for a number of conditions; they reduce side effects, keep drug levels stable, and control the release of cannabinoids. Rubbing CBD oil on the skin can ease arthritis, muscle and joint pain. Cannabis salves, lotions, and ointments effectively treat most skin conditions (burns, itching, infections, and rashes). However, transdermal cannabinoid studies using hairless guinea pigs showed it was difficult to get a high enough plasma level to resolve systemic problems.8
Endogenous cannabinoid deficiency can result from not having sufficient cannabinoid receptors, or from not enough of either or both of the two known endocannabinoids – anandamide and/or 2-AG. An individual’s need for and ability to produce an endocannabinoid will vary, depending on congenital factors, age, activity level, general health, diet, substance abuse, environmental challenges, and, almost always, the inability to adjust to chronic stress. Chronic stress exhausts endocannabinoid tone; when the endocannabinoid system is broken, physiological problems follow.9
In a landmark paper, “Clinical endocannabinoid deficiency (CECD): can this concept explain therapeutic benefits of cannabis in migraine, fibromyalgia, irritable bowel syndrome and other treatment-resistant conditions?,” University of Washington neurologist Ethan Russo postulated that “clinical endocannabinoid deficiency” was the underlying factor in migraines, fibromyalgia, irritable bowel disease, and a cluster of other degenerative conditions. He observed that many recalcitrant neurotransmitter diseases (pathological conditions) were due to systemic deficiencies: Alzheimer’s disease is marked by loss of acetylcholine activity, Parkinson’s disease is due to dopamine deficiency, and depression follows lowered levels of serotonin, norepinephrine or other amines. Russo then questioned whether a clinical endocannabinoid deficiency (CECD), either congenital or acquired, could explain the etiology behind migraine headaches, fibromyalgia, and irritable bowel syndrome, conditions which are all characterized by hyperalgesia, an abnormal sensitivity to pain out of proportion to any underlying causation. And if the cause were endocannabinoid deficiency, could cannabinoid therapy correct the imbalance?9
Fast forward to 2016. Russo’s most current paper, “Clinical Endocannabinoid Deficiency Reconsidered: Current Research Supports the Theory in Migraine, Fibromyalgia, Irritable Bowel, and Other Treatment-Resistant Syndromes,” documents a wealth of studies that support his hypotheses from 2004. Not only did he find that fibromyalgia, migraine, and irritable bowel syndrome shared comorbidity, they had a unified set of pathophysiological conditions:
- All manifest hyperalgesic states [that] must be clinically diagnosed based on subjective criteria as all lack characteristic tissue pathology or easily accessible, objective laboratory findings;
- All are diagnoses of exclusion that often generate extensive negative diagnostic work-ups;
- They display elevated incidence of anxiety and depression…and have been labeled psychosomatic in origin or worse, wastebasket diagnoses, at one time or another by skeptical clinicians;
- Comorbidity is quite clear in the three diagnoses. Primary headaches co-occurred in 97% of 201 fibromyalgia patients; 35.6% of chronic daily headache subjects also fit clinical criteria of fibromyalgia, 31.6% of IBS subjects were also diagnosable with fibromyalgia and 32% of fibromyalgia patients also fit for IBS.
- While some patients suffer from only one of these syndromes, lifetime risk to develop another or all three is quite common.10
Other disorders that may fall under the CECD rubric include neonatal failure to thrive, cystic fibrosis, causalgia, brachial plexopathy, phantom limb pain, infantile colic, glaucoma, dysmenorrhea, neremesis gravidarum, unexplained fetal wastage (repetitive miscarriages), post-traumatic stress disorder, bipolar disease, and possibly many others.10
Where Russo had merely questioned the idea of endocannabinoid deficiency 15 years prior, he now had data. One study, which compared the cerebrospinal fluid of 15 migraine sufferers versus twenty controls, showed phenomenal, statistically significant differences in endogenous cannabinoid system chemicals. Migraine attacks are correlated with depletion of beta endorphins in the central nervous system and extremely low levels of the endogenous cannabinoid, 2-AG.10
To validate Russo’s endocannabinoid hypothesis, a cannabis-oriented clinic in Colorado recommended cannabis prophylaxis for 120 migraine sufferers. Headache frequency dropped from 10.4 to 4.6 headaches per month, 85 percent of the sufferers had fewer headaches, 19.8 percent reported that headaches had been prevented or reduced in intensity, with 11.6 percent of the headaches aborted.10 Another study, this one comparing the effectiveness of cannabis against standard pharmaceutical fibromyalgia treatments, favored cannabis over the “poorly effective prescription medicines.”10
Studies over the past decade have proven the effectiveness of cannabis for ameliorating difficult-to-treat conditions. Russo noted that some problems may not be the result of an absolute endocannabinoid deficiency; imbalances between the endogenous cannabinoids could also cause problems. Russo supports integrating lifestyle approaches to the endocannabinoid support regimen, including dietary manipulations with probiotics and prebiotics to enhance health.10
Now almost 80 years after the illegalization of cannabis, we still have minimal or no cannabinoids in our food or medicines. Many of us suffer a variety of conditions that researchers have linked to cannabinoid deficiency – although it is not for lack of cannabinoids in our diets that we are afflicted with endocannabinoid deficiency. Endo- refers to the cannabinoids our bodies produce – not the ones we eat. So, if eating is involved, we may not be eating the right “building blocks.” Our endocannabinoid deficiency is probably more a result of chronic stress, physiological and environmental factors, and a diet far removed from that which sustained our forefathers–which was probably not particularly healthy most of the time, but at least it was real food.
When human beings get even a little sun exposure, they manufacture vitamin D. What if we were missing some chemical link so that our vitamin D “factory” were broken? Wouldn’t it make sense to supplement our diets with a vitamin D tablet or vitamin D fortified food?
Page 1, 2
Retrieved from: http://www.townsendletter.com/Nov2017/cannabinoid1117.html